Malaria Risk Africa Travel 2026: Why It Still Threatens Travelers
Malaria risk across Africa remains one of the most significant travel health considerations in Southern and East Africa in 2026. Understanding Malaria Risk Africa Travel 2026 is essential for anyone planning visits to high-risk zones. While medical research, vaccine development, and prevention campaigns continue to advance, malaria still affects millions of people annually, particularly in coastal regions, river basins, low-lying tropical areas, and certain wildlife destinations.
Travellers often underestimate the seriousness of malaria because many safari and beach regions feel well developed and tourism-ready. However, mosquito exposure does not correlate with hotel quality. Risk depends on geography, altitude, rainfall patterns, and seasonality. In parts of Mozambique, Tanzania, Kenya, Zambia, and Zimbabwe, malaria remains present in specific regions, particularly near lakes, floodplains, and coastal districts. Even in South Africa, risk exists in limited northern areas during certain seasons.
A critical misunderstanding among international travellers is timing. Malaria symptoms can appear days or even weeks after exposure, sometimes after returning home. Fever, chills, headaches, fatigue, muscle pain, and flu-like symptoms should never be ignored if recent travel included a malaria-risk area. Immediate testing is essential, as delayed treatment increases complication risk.
This updated malaria guide outlines key insights for Malaria Risk Africa Travel 2026 planning. It explains how regional risk levels differ, how rainfall and temperature influence mosquito density, and why altitude significantly reduces exposure in certain destinations. It details prevention strategies including prophylactic medication consultation before departure, insect repellent use, long-sleeved evening clothing, mosquito netting, and accommodation screening practices.
It also emphasizes immediate testing requirements. Any unexplained fever after visiting a risk area should trigger urgent malaria screening, even if prophylaxis was taken. No prevention method is 100 percent protective.
TravelSafe SOS supports travellers across 17 countries in Southern and East Africa by providing coordinated assistance when symptoms arise. The app connects users to vetted private clinics, facilitates rapid referral for testing, and ensures communication with insurers and family members if hospitalization or evacuation becomes necessary. In remote safari or coastal regions, centralized coordination reduces delays that can critically affect outcomes.
Malaria remains manageable with awareness, prevention, and rapid response. In 2026, informed planning, early symptom recognition, and access to structured support systems are the foundation of safe travel in malaria-risk regions of Africa.
Disclaimer: This article is for informational purposes only. It does not replace medical advice. If you feel unwell, contact a healthcare professional immediately.
Where Malaria Risk Is Highest in Southern and East Africa in 2026
Malaria risk levels across Africa vary significantly by geography, altitude, rainfall, and seasonal mosquito breeding cycles. Transmission typically peaks from November to May in Southern Africa and from March to June in parts of East Africa, following heavier rainfall patterns. Even experienced travellers and field professionals can be caught off guard when exposure coincides with peak mosquito activity.
Within our own operational teams working across Mozambique, Tanzania, Zambia, and Malawi, malaria infections have occurred despite strong awareness. In every case, rapid testing and immediate treatment were decisive in preventing serious complications. Speed matters.
Key high-risk areas by country in 2026 include:
• Mozambique, high risk countrywide, particularly along the coastline, Zambezi Valley, Gorongosa, Niassa, and the Bazaruto Archipelago
• Malawi, high risk around Lake Malawi, Liwonde, Majete, and rural districts
• Zambia, Luangwa Valley, Kafue, Lower Zambezi, and western wetland regions
• Zimbabwe, high risk in Victoria Falls, Mana Pools, Kariba, and the Zambezi Valley
• Botswana, northern Botswana shows seasonal malaria patterns including Chobe and the Okavango Delta
• Namibia, Zambezi Region and parts of Kavango remain elevated risk zones
• Tanzania, coastal regions, Zanzibar, Selous, Ruaha, and remote reserves
• Kenya, coastal belt including Mombasa and Lamu, Lake Victoria Basin, Kisumu, and Kakamega
• Uganda, widespread presence, particularly rural and forested areas
• Rwanda, lower overall risk but caution required in certain rural lakeside districts
• South Africa, low national risk, though Kruger National Park, Limpopo, and Pafuri require prophylaxis during peak seasons
It is important to recognize that luxury accommodation does not eliminate malaria exposure. Mosquitoes do not distinguish between budget and high-end properties. Risk increases during evening game drives, river cruises, walking safaris, and visits to lakeside or village areas where mosquito density may be higher.
Prevention strategies must therefore be layered: medical consultation for prophylaxis before departure, consistent use of repellents containing appropriate active ingredients, long-sleeved clothing at dusk, screened or netted sleeping environments, and immediate testing if symptoms arise.
Malaria in 2026 remains manageable with vigilance, but it is not negligible. Awareness of regional variation and seasonal peaks is fundamental to responsible travel planning across Southern and East Africa.
If you are planning a longer trip, always be aware of malaria symptoms and act immediately. If in doubt – the first rule is seeking treatment. Speak to your travel doctor before travel and if recommended by them, besides your prophylactics – carry a dose of Coartem or similar malaria treatment with you. Remember, just because you have been tested and the result is negative, it doesn’t mean you don’t have malaria. You may also arrive at a health facility and test positive, but they have no treatment options available.
These patterns shape what travelers must prepare for under Malaria Risk Africa Travel 2026 guidelines.
Malaria Symptoms During and After Travel: What to Watch For
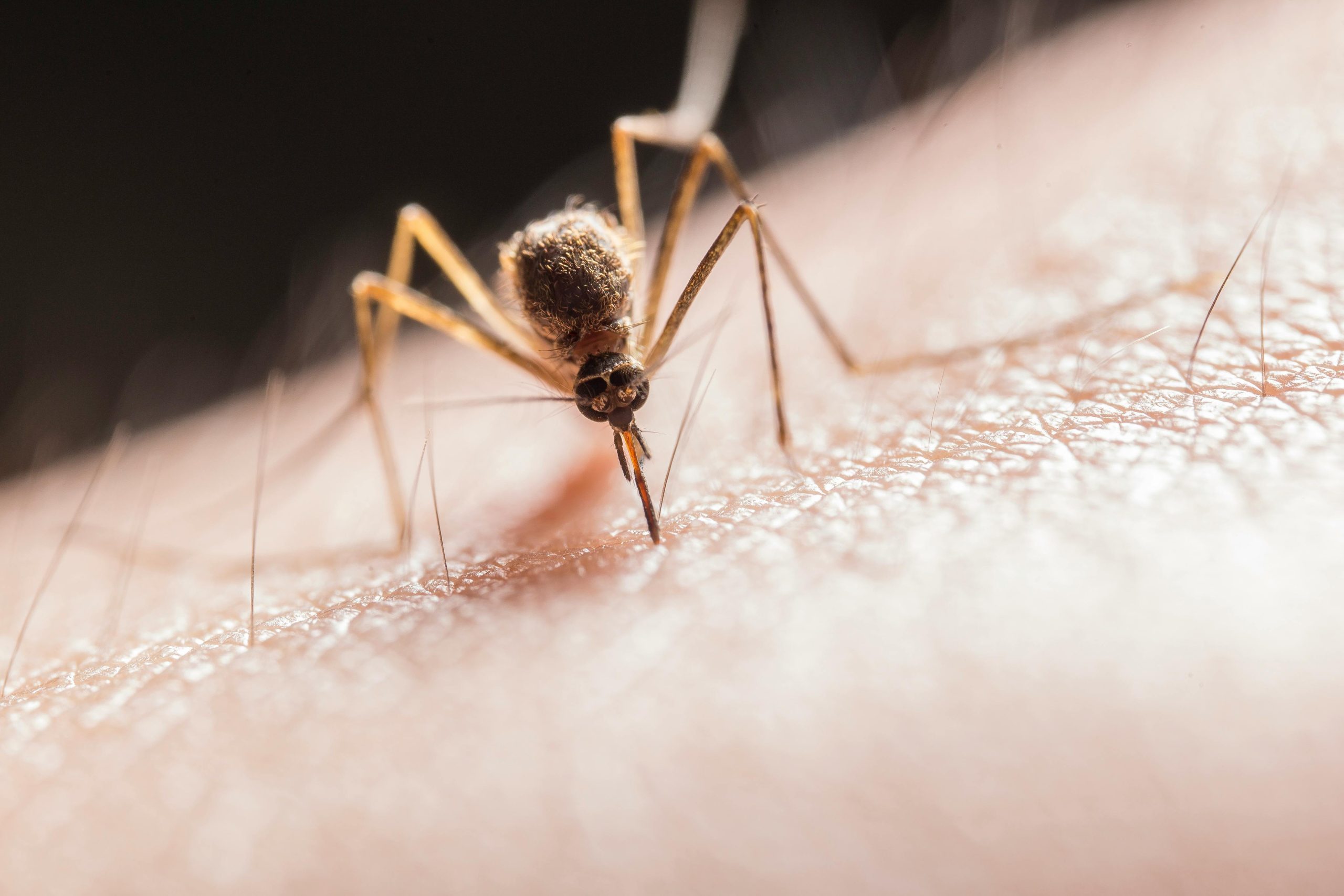
Malaria often begins like a mild viral illness, which is why travelers overlook it. The disease is caused by Plasmodium parasites transmitted by the female Anopheles mosquito. Recognizing signs early is vital for reducing danger under Malaria Risk Africa Travel 2026, especially if symptoms appear after returning home
Common early signs include:
• Fever or chills
• Headache, fatigue, or weakness
• Muscle pain or joint soreness
• Nausea or diarrhoea
• Dizziness or faintness
• Night sweats
• A dry cough or shortness of breath
Symptoms may start 7 to 14 days after exposure—or even later, particularly with P. falciparum, the most dangerous strain found across this region. Some cases only present after returning home, which is why prompt testing is essential if you feel unwell after your trip.
Why Immediate Testing Saves Lives, Including After Returning Home
One of the biggest risks for travelers is delayed diagnosis. Many travelers return to Europe or North America and assume their symptoms are flu, jet lag, or a stomach bug. Testing urgency is one of the core pillars of Malaria Risk Africa Travel 2026, particularly for travelers returning to non-malaria countries. Healthcare professionals in non-malaria countries may overlook malaria unless the traveler insists on being tested.
You must request a malaria test if:
• You have visited a malaria country in the past 30 days
• You develop fever, headache, exhaustion, or unexplained symptoms
• You are pregnant, immunocompromised, or traveling with children
• Your symptoms do not match a typical viral illness
Misdiagnosis leads to serious complications, hospitalization, or worse. If you feel unwell or are unsure, ask your doctor for a blood smear or rapid diagnostic test (RDT). Always tell them exactly where you travelled.
Why Clinics Outside Africa Often Miss Malaria Cases
Despite improvements in global healthcare, the malaria risk in Africa remains high and malaria remains an unfamiliar disease to many general practitioners in Western countries. In emergency rooms or family practices, few clinicians immediately suspect malaria unless you mention it—and even then, some may dismiss it due to low prevalence in their region.
If you suspect malaria:
- Ask for a blood smear or rapid diagnostic test (RDT)
- Mention your travel destination and exposure to mosquito-prone zones
- Do not accept a broad viral diagnosis if symptoms persist without explanation
The TravelSafe SOS app provides vital guidance while still in Africa. If symptoms arise on your trip, the app connects you with trained paramedics who can assess your condition and coordinate testing, treatment, or evacuation.
How to Prevent Malaria in 2026: Essential Traveler Practices
Prevention requires a combination of medication and mosquito avoidance.
Recommended prophylaxis (speak to your doctor first):
• Atovaquone Proguanil, Daily, widely used
• Doxycycline, Effective and inexpensive but causes sun sensitivity
• Mefloquine, Weekly, but potential mood or sleep side effects
Medication should begin before entering a malaria zone, continue daily during travel, and be completed after returning home.
Mosquito prevention:
• Apply 30 percent DEET repellent from sunset
• Wear long sleeves and light trousers in the evenings
• Sleep under treated mosquito nets
• Stay in screened or air conditioned rooms
• Avoid outdoor lighting that attracts mosquitoes
Who Faces the Highest Malaria Risk in Africa
Some travelers need enhanced protection:
• Children
• Pregnant women
• Older travelers
• Immunocompromised travelers
• Solo travelers in remote areas
• Backpackers or overlanders on multi day routes
The TravelSafe SOS app monitors your emergency, guides you to care, and supports evacuation if symptoms escalate.
Malaria Risk in Africa: Who Needs Extra Protection?
Some travelers are especially vulnerable to serious malaria complications:
- Children: Lack fully developed immunity, symptoms can escalate fast
- Pregnant women: Higher risk of severe illness or miscarriage
- Older adults: May show non-specific symptoms like confusion or fatigue
- Solo travelers or remote explorers: May not have immediate access to care
The TravelSafe SOS app ensures that even if you’re alone or far from help, a control center will monitor your emergency and guide you to care. The app is your bridge between local knowledge and expert medical advice across the entire region.
What to Do If Malaria Symptoms Appear While Traveling
If you’re traveling in any covered country and feel unwell:
- Tap the SOS button in the TravelSafe SOS app
- Speak to the control center paramedic who will assess your condition
- Get directed to the nearest trusted clinic for testing and treatment
- If required, receive evacuation assistance to a more advanced hospital
- Your travel agent, insurer, and emergency contact will be automatically notified
Do not try to self-medicate or wait until your next destination. Malaria can worsen dramatically in 24–48 hours. Early intervention saves lives. Take it very seriously.
Malaria Symptoms After Returning Home: What To Do
Many travelers let their guard down once they return to Europe or North America. But if symptoms show up, act immediately.
- Don’t assume it’s jet lag, flu, or food-related.
- Don’t wait to “see if it passes.”
- Don’t rely on generic antibiotics or self-treatment.
Request malaria testing, even if you were taking prophylactics. Although rare, breakthrough cases do occur. Mention specific locations you visited, especially high-risk zones like Victoria Falls, Lake Malawi, or Zanzibar.
Why a Travel Safety App Matters for Malaria Awareness
TravelSafe SOS does not diagnose malaria, but it provides the real time support required to get you to proper medical care. If you are in a remote safari area or a coastal island with limited medical facilities, the app ensures that responders know where you are, what symptoms you have, and how urgently you need help. This reduces delays in accessing testing and treatment, which is critical for malaria survival.
Final Takeaway: Managing Malaria Risk Africa Travel 2026
With proper planning and awareness of Malaria Risk Africa Travel 2026, travelers can safely enjoy Southern and East Africa. Malaria remains a serious but manageable travel risk. With the correct prevention and fast access to testing, you can travel safely throughout Southern and East Africa. Use prophylaxis, apply mosquito protection, monitor symptoms, test immediately, and rely on the TravelSafe SOS app for emergency coordination.
Disclaimer
This article is not intended to replace professional medical care. Always consult your doctor before travel and seek licensed clinical help if you feel unwell. TravelSafe SOS provides coordination and communication support—not diagnosis or treatment.
FAQs - Malaria Risk in Africa Travel 2026
Do I still need malaria prevention medication for Africa in 2026?
Yes. Despite vaccine progress, malaria remains widespread in many African regions. Travelers visiting Mozambique, Tanzania, Zambia, Malawi, Kenya, and Uganda still need antimalarial medication. Your doctor will advise the right prophylaxis. Medication must begin before travel and continue after returning home.
How fast do malaria symptoms appear after a trip to Africa?
Symptoms can appear 7 to 14 days after infection, but some travelers fall ill weeks later. If you have fever, chills, fatigue, or severe headache after returning home, request immediate malaria testing. Mention all countries you visited because late recognition leads to delayed treatment.
Which countries in Africa have the highest malaria risk for tourists in 2026?
High risk continues in Mozambique, Malawi, Zambia, Zimbabwe, Tanzania, Zanzibar, Uganda, and Kenya. Northern Botswana and Namibia’s Zambezi Region also have seasonal outbreaks. South Africa has low risk, but Kruger and northern Limpopo require prophylaxis.
Can I still get malaria even if I took prophylaxis correctly?
Yes, breakthrough infections are uncommon but possible. Prophylaxis reduces the risk and severity, but it does not eliminate all risk. If you feel unwell after travel, request malaria testing immediately even if you completed your medication.
What should I do if I think I have malaria while on safari?
Use the TravelSafe SOS app to contact the control center, explain symptoms, and receive instructions on where to test. The paramedic team will guide you to a clinic or coordinate evacuation if necessary. Speed of response is essential.
Is malaria common in Zanzibar and Tanzanian islands in 2026?
Yes, Zanzibar still has malaria risk, although lower than mainland Tanzania. Travelers should take prophylaxis and use mosquito protection. Island resorts use prevention measures, but exposure increases on tours, dhow trips, and village visits.
How does a travel safety app help with malaria emergencies?
A travel safety app provides immediate human support, helps identify symptoms, alerts responders, coordinates testing, and notifies your insurer and family. If you are far from medical care, this rapid coordination can prevent life threatening delays.